Transposition of the
Great Vessels
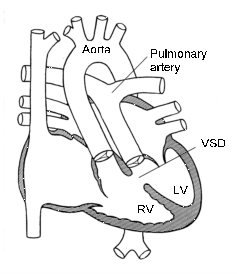 In this congenital heart
defect, the aorta (the main artery that carries blood to the body) originates
from the right ventricle and the pulmonary artery (the artery that carries low
oxygen blood to the lungs) from the left ventricle, resulting in two separate
circulation’s.
In this congenital heart
defect, the aorta (the main artery that carries blood to the body) originates
from the right ventricle and the pulmonary artery (the artery that carries low
oxygen blood to the lungs) from the left ventricle, resulting in two separate
circulation’s.
Because the great arteries are reversed,
the aorta carries blood from the right ventricle. This low oxygen rich blood and
likewise the pulmonary artery carries blood from the left ventricle. This is
already oxygen rich blood that is being carried back to the lungs. In order for
the infant born with transposition of the great arteries to survive, they must
have some communication between the right and the left sides of the heart to
allow oxygen rich blood to reach the body. This mixing of blood is possible
through any of the following: ASD, VSD, PDA. Even though there is mixing of
oxygenated and de-oxygenated blood, it is often not adequate to sustain life for
an extended period of time. Babies with transposition are extremely blue at
birth.
The most common surgical procedure to
correct this defect is called an arterial switch operation. That is, the major
arteries are "switched". The aorta is connected to the left ventricle. This
allows oxygen rich blood to be pumped to the body. The pulmonary artery is
connected to the right ventricle. This allows low oxygen blood to go to the
lungs where it can be oxygenated. Other surgical defects may also be needed to
correct the communication between the left and right sides of the heart that was
once needed for survival.
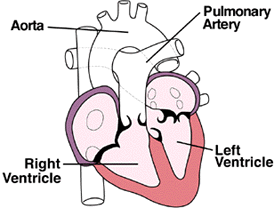 |
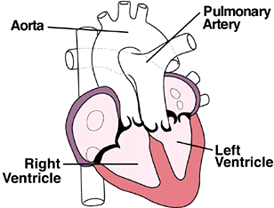 |
| Normal |
Transposition |
In this situation, the
pulmonary arteries are supplied by the left ventricle, and the aorta by the
right ventricle. This, of course, is the opposite of the normal arrangement.
Infants can only survive if there is a shunt between the two sides of the heart,
and an atrial septal defect needs to be actually enlarged to allow adequate
mixing of blood to deliver enough oxygenated blood to the body. Significant
advances have been made in the surgical treatment of this disorder.

Illustrations
|
 |
 |
 |
|
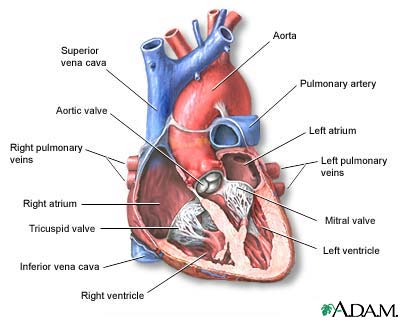
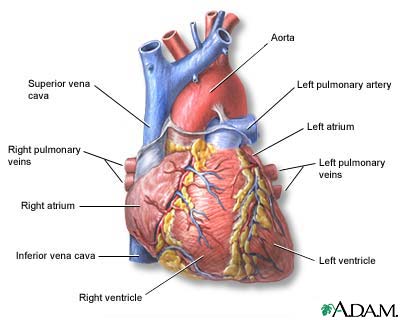
The interior of the heart is composed of
valves, chambers, and associated vessels. |
The external structures of the heart include the
ventricles, atria, arteries and veins. Arteries carry blood away from the
heart while veins carry blood into the heart. The vessels colored blue
indicate the transport of blood with relatively low content of oxygen and
high content of carbon dioxide. The vessels colored red indicate the
transport of blood with relatively high content of oxygen and low content of
carbon dioxide. |
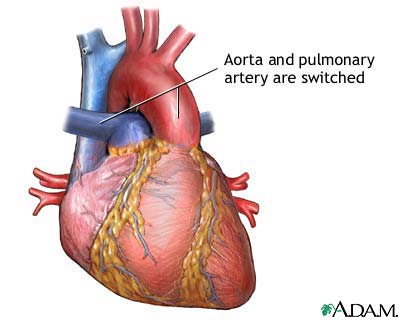
Transposition of the great vessels is a congenital
heart defect in which the position of the two major vessels that carry blood
away from the heart - the aorta and the pulmonary artery - is switched
(transposed). This defect is classified as a cyanotic heart defect because
the condition results in insufficiently oxygenated blood pumped to the body
which leads to cyanosis (a bluish-purple coloration to the skin) and
shortness of breath. |
Alternative names
Return to top
Transposition of the great arteries
Definition
Return to top
Transposition
of the great vessels is a congenital heart defect in
which the 2 major vessels that carry blood away from the heart -- the aorta and
the pulmonary artery -- are switched (transposed).
Causes, incidence, and risk factors
Return to top
The cause of most congenital heart
defects is unknown. Prenatal factors associated with a higher than normal
incidence of these disorders include maternal rubella or other viral illnesses
during pregnancy, poor prenatal nutrition, maternal alcoholism, maternal age
over 40, and diabetes, although it is unclear if any of these actually cause the
problem.
Transposition
of the great vessels is classified as a cyanotic heart
defect because the condition results in insufficiently oxygenated blood pumped
to the body which leads to cyanosis (a bluish-purple coloration to the skin) and
shortness of breath.
In
transposition of the great
vessels, there is no communication between the pulmonary circulation and the
systemic circulation. Fresh oxygenated blood from the lungs returns to the heart
ready to nourish the body, but instead is whisked right back to the lungs.
Conversely, oxygen-poor blood returns from the body to the heart and is then
sent right back out to the body without being reoxygenated. There is usually an
associated defect that permits the mixing of the systemic and pulmonary
circulation to provide some oxygenated blood to the body. Without such a defect,
the condition is rapidly fatal.
Symptoms appear at birth or very soon
afterwards. The severity of the symptoms depends upon the type of associated
defect and the resulting amount of oxygenated blood supplied to the general
circulation. The condition affects approximately 40 out of 100,000 infants. It
is the most common cyanotic heart defect identified in the first week of life.
Symptoms
Return to top
- Blueness of the skin
- Shortness of breath
- Poor feeding
- Clubbing of the fingers or toes
Signs and tests
Return to top
The health care provider may detect a
heart murmur while listening to the chest with a stethoscope.
Tests often include the following:
- Chest x-ray
- Cardiac catheterization
- ECG
- Echocardiogram
Treatment
Return to top
Immediately after diagnosis, a medication
called prostaglandin is started intravenously to maintain the small connection
(the ductus arteriosus) between the pulmonary and systemic circulations. Surgery
to temporarily adjust the vessels may be required shortly after birth, with
permanent correction postponed until the child is older. However, a surgical
technique known as an arterial switch procedure allows permanent correction
within the first month of life.
Expectations (prognosis)
Return to top
Improvement in symptoms and growth and
development is seen after surgical correction of the defect. If corrective
surgery is not performed, the life expectancy is shortened.
Complications
Return to top
- Arrhythmias
- Heart valve problems
Calling your health care provider
Return to top
This condition is usually diagnosed when
a baby is born. Go to the emergency room or call the local emergency number such
as 911 if your baby's skin develops a bluish color.
Call the health care provider if your
baby has this disorder and new symptoms develop, become worse over time, or if
symptoms continue after treatment.
Prevention
Return to top
Women who plan to become pregnant should
be immunized against rubella if they are not already immune. Good nutrition,
avoiding alcohol, and control of diabetes both before and during pregnancy may
be helpful.
 In this congenital heart
defect, the aorta (the main artery that carries blood to the body) originates
from the right ventricle and the pulmonary artery (the artery that carries low
oxygen blood to the lungs) from the left ventricle, resulting in two separate
circulation’s.
In this congenital heart
defect, the aorta (the main artery that carries blood to the body) originates
from the right ventricle and the pulmonary artery (the artery that carries low
oxygen blood to the lungs) from the left ventricle, resulting in two separate
circulation’s.



